Neurotrophic keratitis can be a frustrating and potentially debilitating disease for patients, thus early diagnosis and targeted treatment are critical. While it’s a challenging disease to treat, just making the diagnosis comes with its own set of challenges. We can only diagnose what we’re aware of and what we’re looking for, and finding the proper treatment for any disease is difficult if we’re not well informed of the treatment options.
Here, I share an overview of this vision-threatening disease and several cases illustrating the variety of clinical presentations and treatment strategies that are possible.
Etiologies and Comorbidities
The etiologies of neurotrophic keratitis can be divided into four categories: ocular, systemic, central nervous system, and genetic (Figure 1).1,2 Not all of these conditions lead to neurotrophic keratitis, but when we see someone with contact lens-related disorders, for example, or severe dry eye that is unresponsive to treatment, we need to consider the possibility that the patient has a neurotrophic cornea.

Because our tertiary care facility is located one floor above a cancer center, we see many patients with graft-versus-host disease, a common underlying problem that can lead to neurotrophic keratitis. Whenever we see comorbidities, such as limbal stem cell deficiency or exposure or radiation keratopathy, we need to ask ourselves if the innervation to the cornea is normal or abnormal. Even chronic eye rubbing, which is common among patients who have keratoconus, can lead to a neurotrophic cornea over time.
Prevalence and Risk Factors
Neurotrophic keratitis is classified as a rare disease, as it affects fewer than 65,000 people in the United States. Despite this classification, neurotrophic keratitis doesn’t seem so rare in my practice. As a cornea physician, I estimate that at least 10 of the 50 patients I see in a day have neurotrophic keratitis.
To gain a sense of the overall prevalence of at-risk patients, I identified the four most common types of patients diagnosed with neurotrophic keratitis in my clinic and researched the incidence in the United States.3-6 Consider the following:
- More than 10% of our population has diabetes.3
- HSV keratitis is also a common entity.4 I see at least five or six cases a day.
- Roughly 10 million Americans have had LASIK surgery since its approval in 1999,5 and many of these patients are developing age-related diseases.
- Glaucoma affects 2.7 million individuals who are 40 years of age or older in the United States.6
The risk of neurotrophic keratitis increases exponentially when patients present with complicated histories that include more than one of these risk factors.
Diagnosis and Disease Staging
Devising a proper treatment strategy for patients with neurotrophic keratitis requires a three-step diagnostic process, starting with a detailed clinical history that focuses on detecting underlying issues associated with trigeminal impairment.7
Step two is an assessment of corneal sensitivity. I begin by observing the patient and asking about symptoms. Often, I see a severe problem on the ocular surface that I would expect to be painful, but the patient reports only blurry vision without pain. Next, I perform a fast and simple corneal sensitivity test. I use a wisp of a sterile cotton swab—some clinicians use a small piece of sterile dental floss—to tap the surface of the eye and note the reaction or lack thereof.
Step three, the slit lamp examination, will reveal the presence of epithelial alterations, confluent superficial punctate keratitis, persistent epithelial defects, or corneal ulcers.7 We have many high-tech devices to analyze the eye, but a simple slit lamp examination with fluorescein staining is the basis for making this diagnosis.
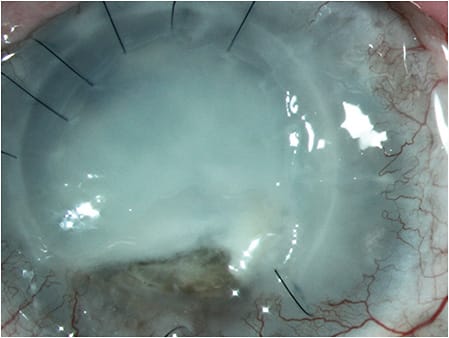
Staging neurotrophic keratitis as mild (punctate epithelial keratopathy), moderate (epithelial defect), or severe (corneal ulcer with stromal involvement) using the Mackie classification enables us to design an appropriate treatment strategy and document disease progression.1,8,9 Once the stroma becomes involved, the patient is at risk for superinfection and perforation (Figure 2).
The following cases illustrate the wide-ranging presentations of neurotrophic keratitis at various stages and the multiple treatment options available.
Case 1: Fluctuating Vision Post LASIK
A 65-year-old woman has a history of scleroderma. She underwent LASIK surgery after having worn rigid gas permeable contact lenses for 40 years. Her chief concern was blurry, fluctuating vision. She noted no foreign body sensation, redness, burning, or ocular pain. Her visual acuity was 20/30 in the right eye and 20/25 in the left eye.
Slit lamp examination revealed dermatochalasis, significant meibomian gland dysfunction (MGD), mild nasal pinguecula, 2+ punctate epitheliopathy, early cataracts, and an elevated cup-to-disc ratio.
The standard screening for ocular surface disease in our clinic includes tear osmolarity, MMP-9, and the Ocular Surface Disease Index questionnaire. These tests are particularly important to perform for patients who will undergo any type of refractive surgery, whether it’s LASIK or cataract surgery. This patient will be undergoing cataract surgery, potentially premium cataract surgery, in the near future.
Despite significant changes visible on the corneal surface (Figure 3), the patient reported no ocular pain or burning. Initial corneal topography showed areas of elevation and depression (Figure 4, top). After 3 months of treatment with topical cyclosporin, low-dose steroids, frequent preservative-free tears and lid hygiene (Figure 4, bottom), the topography was much improved.
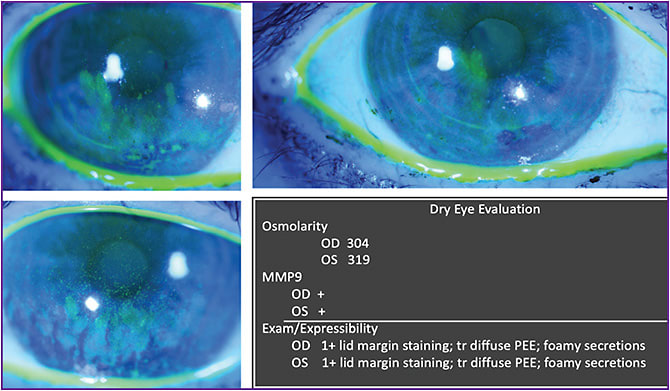
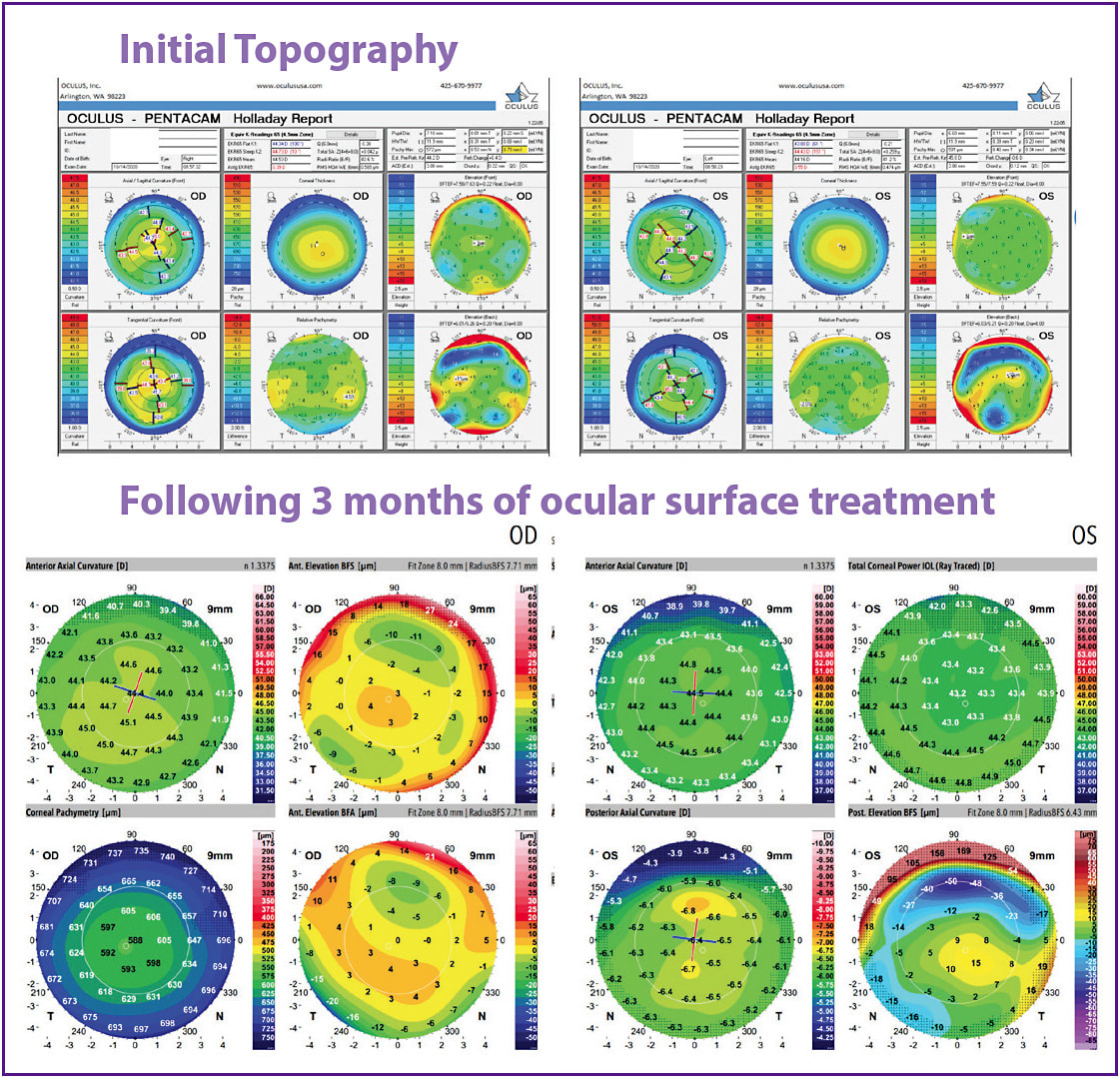
In my experience, patients really become interested in partnering with us in their treatment when they understand the images that we’re sharing with them at repeat examinations. Fortunately, with today’s technology, we can help them visualize what the problem is and how treatment is helping them.
Case 2: HSV Keratitis
A 60-year-old woman has a long history of HSV keratitis in her right eye. Her visual acuity is 20/60 in her right eye and 20/100 in her left eye, which is amblyopic. She reported extreme fluctuations in vision with her right eye but noted no pain. She has early cataracts that are not visually significant.
The patient was previously treated with a steroid for epithelial keratitis, which resolved, and she had been treated with ganciclovir ophthalmic gel (Zirgan, Bausch + Lomb) in the past.
When I saw the patient, she was using fluorometholone acetate (Flarex, Alcon) in her right eye and serum tears—an excellent adjunctive therapy—in both eyes. To this regimen, I added cenegermin-bkbj (Oxervate, Dompé), which is the only medication approved for the treatment of neurotrophic keratitis.
Figure 5 shows the patient’s right eye before treatment with cenegermin-bkbj. What appears to be an active dendrite is actually residual scarring within the corneal stroma due to a series of multiple episodes of recurrent keratitis through the years.
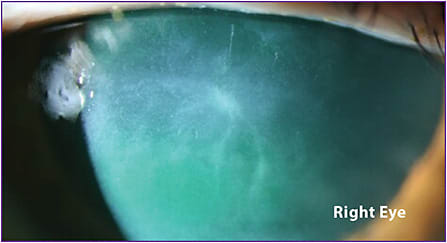
Over an 8-week course of treatment with cenegermin-bkbj, the neurotrophic keratitis improved significantly. We continued the serum tears and topical lubricants.
Case 3: HSV, Diabetes, Rosacea, and Eczema
This 37-year-old man has HSV and uncontrolled type 1 diabetes. He has diabetic retinopathy, which is being monitored by the retina service, and he is being treated in our dermatology department for severe rosacea and eczema.
Clinical examination revealed 3+ MGD, diffuse limbal vascularization, stromal scarring in both eyes, and a nonhealing central epithelial defect in the left eye. The patient noted no ocular pain or foreign body sensation.
The patient had been treated for epithelial disease from his HSV keratitis and for the more chronic stromal disease. He was using acyclovir, as well as aggressive artificial tears, gels, and warm compresses. I prescribed cenegermin-bkbj six times a day.
Figure 6 shows where chronic dendrites have resolved with the chronic limbal vascularization, which at one point had spread across the entire cornea of the left eye. The steroid aided vascular regression, but the patient has struggled with some recurrences. The patient’s visual acuity is now 20/30 in his right eye and 20/50 in his left eye.
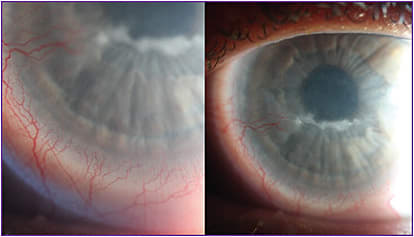
Case 4: Systemic Autoimmune and Inflammatory Disease
This 65-year-old man has severe rheumatoid arthritis and a history of bilateral retinal detachments, bilateral silicone oil, with history of vitrectomy and bilateral silicone oil, with a scleral buckle on the left eye. He’s had multiple amniotic membranes placed after perforations.
The patient has a long history of noncompliance with prescribed medications, including methotrexate and oral prednisone, and he has repeatedly been lost to follow-up over a period of years. His vision is counting fingers in both eyes.
The patient has experienced perforations in both eyes. Figure 7 (top) shows the right eye when the patient had a descemetocele and (bottom) after amniotic membrane placement to treat the thinning cornea. The patient has received multiple amniotic membranes and several courses of cenegermin-bkbj.
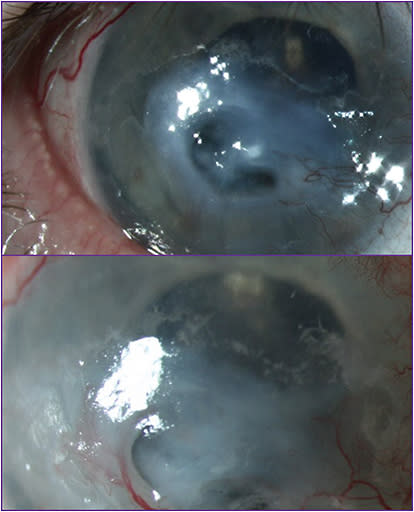
Patients with systemic autoimmune and inflammatory diseases can be particularly challenging to diagnose and treat. It’s important to check corneal sensation in both eyes, as these patients likely have bilateral neurotrophic keratitis.
Case 5: Long-Term Topical Antiglaucoma Therapy
This 64-year-old man has a 20-year history of primary open-angle glaucoma treated with topical antiglaucoma medications. Recently, his IOP has been adequately controlled, but that has not always been the case. He is using brimonidine, dorzolamide hydrochloride-timolol maleate (Cosopt, Merck & Co., Inc.), latanoprost (Xalatan, Pfizer), and aggressive artificial tears. While wearing a bandage contact lens, he uses polymyxin.
The patient has experienced bilateral retinal detachments, and he has undergone multiple retina surgeries in the right eye. He has no sensation in his right eye and was diagnosed with neurotrophic keratitis. The patient completed two courses of cenegermin-bkbj.
Figure 8 shows stage one neurotrophic keratitis with diffuse punctate epitheliopathy. While the disease advanced to stage two at times, it never reached stage three.
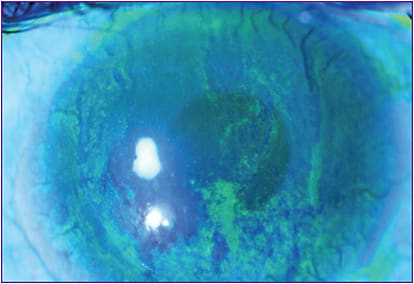
Because of the toxicity associated with some topical antiglaucoma medications, we should suspect neurotrophic keratitis in any of these long-term glaucoma patients, particularly those who have severe disease and are using three or four topical medications.
Summary
The hallmark of neurotrophic keratitis is signs and symptoms that don’t correlate. Patients with a history of contact lens wear, LASIK, cataract surgery, or glaucoma surgery are particularly at risk of developing neurotrophic keratitis, which becomes more challenging to treat later in the course of the disease. Strive to intervene as early as possible to halt the progression of the disease.
Cataract and refractive surgeons need to be alert for neurotrophic keratitis preoperatively. If the disease is not diagnosed and treated prior to surgery, patients may believe their surgery created this condition.
Treatments for neurotrophic keratitis are typically prescribed according to disease severity, but they are not mutually exclusive of one another. For stage one, we typically begin with topical agents—artificial tears, corticosteroids, serum tears, antibiotics, and cenegermin-bkbj. I recommend prescribing cenegermin-bkbj early in the course of neurotrophic keratitis rather than waiting until it progresses. Dompé has a program available to assist patients in acquiring cenegermin-bkbj, and it usually takes about one week to gain access to that medication. I also advise treating patients with serum tears early in the disease course before the scarring and vision problems commonly seen in stage three become permanent.
In-office therapies include bandage contact lenses, punctal occlusion, nonsurgical eyelid closure, amniotic membrane, and tissue adhesive agents. Surgical interventions include therapeutic penetrating keratoplasty, conjunctival flap procedures (such as a Gunderson flap), and various types of sutured amniotic membranes.
In Closing
Neurotrophic keratitis is a degenerative corneal disease characterized by impaired trigeminal innervation.9 Numerous etiologies in addition to herpes simplex and herpes zoster can lead to neurotrophic keratitis, including long-term contact lens wear, ocular surgeries, diabetes, stroke, and toxicity associated with topical medications.1,2
Awareness of the disease and implementation of corneal sensitivity testing are fundamental to the diagnosis and treatment of neurotrophic keratitis.2,8 I really encourage you to look for it in your clinic. I think you’ll be surprised to find it’s more prevalent than you may have thought. Timely diagnosis and treatment gives these patients relief, stabilizes their vision, and prevents some of the sequelae that can be so characteristic of neurotrophic keratitis.
References:
- Sacchetti M, Lambiase A. Diagnosis and management of neurotrophic keratitis. Clin Ophthalmol. 2014;8:571-579.
- Dua HS, Said DG, Messmer EM, et al. Neurotrophic keratopathy. Prog Retin Eye Res. 2018;66:107-131.
- Centers for Disease Control and Prevention. National Diabetes Statistics Report, 2020. Atlanta, GA: Centers for Disease Control and Prevention, U.S. Dept of Health and Human Services; 2020.
- Xu F, Sternberg MR, Kottiri BJ, et al. Trends in herpes simplex virus type 1 and type 2 seroprevalence in the United States. JAMA. 2006;296(8):964-973.
- Rogers C. LASIK: Know the Rewards and the Risks. WebMD Health News. https://www.webmd.com/eye-health/news/20180727/lasik-know-the-rewards-and-the-risks . Published July 27, 2018; Accessed May 10, 2021.
- National Eye Institute. Glaucoma Data and Statistics. https://www.nei.nih.gov/learn-about-eye-health/resources-for-health-educators/eye-health-data-and-statistics/glaucoma-data-and-statistics . Last updated July 17, 2019; Accessed May 10, 2021.
- Mastropasqua L, Nubile M, Lanzini M, Calienno R, Dua HS. In vivo microscopic and optical coherence tomography classification of neurotrophic keratopathy. J Cell Physiol. 2019;234(5):6108-6115.
- Versura P, Giannaccare G, Pellegrini M, Sebastiani S, Campos EC. Neurotrophic keratitis: current challenges and future prospects. Eye Brain. 2018;10:37-45.
- Mastropasqua L, Massaro-Giordano G, Nubile M, Sacchetti M. Understanding the Pathogenesis of Neurotrophic Keratitis: The Role of Corneal Nerves. J Cell Physiol. 2017;232(4):717-724.









